- Home
- Latest News
- News Report Headlines
- Young NI woman ...
Young NI woman given 1% chance of survival after drug abuse urges others to seek help
- News Report Headlines2023-10-23
- Young NI woman given 1% chance of survival after drug abuse urges others to seek help
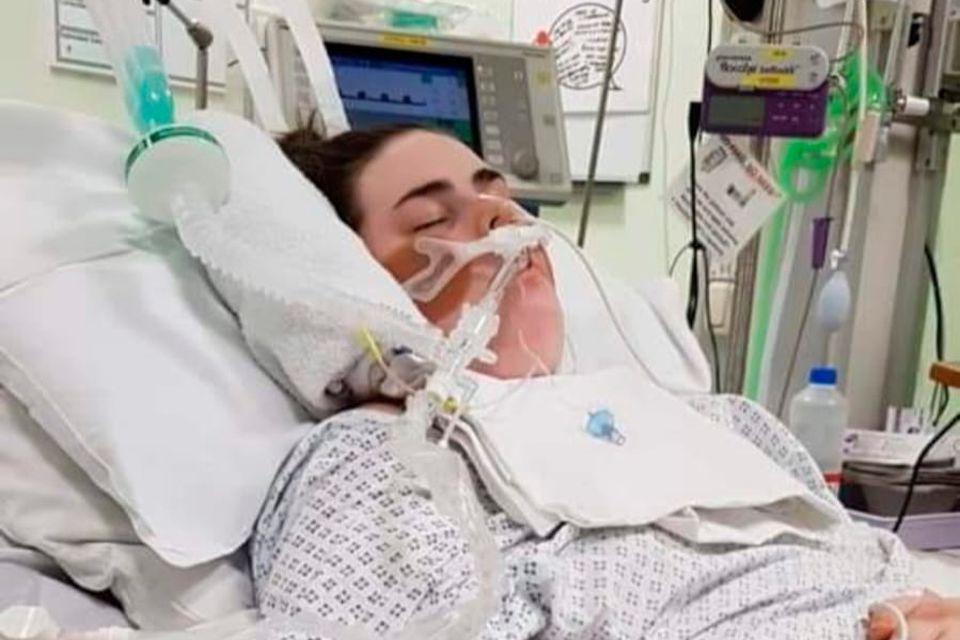
Rachel needed life-saving hospital treatment
A Co Londonderry woman whose “life was changed forever” by substance abuse and now suffers from chronic illness has spoken about the harsh realities of addiction.
Rachel Kordula said drink and drugs drove her to a dark place, and at one stage left her needing life-saving medical care.
She is now determined to use her experience to raise awareness, and is sharing her traumatic story as a warning to others.
Now 24, Rachel described how, on New Year’s Day 2019, she was found lying unconscious by her mother after an overdose.

Now 24, Rachel Kordula wants to warn others of the dangers of substance abuse.
A year before this, aged 18, Rachel had been struggling with her mental health, developing an unhealthy relationship with alcohol. She was introduced to drugs, which she said she used to try to escape from reality.
“The area I was living in at the time was prolific with drugs. It felt completely normal to go out and do that,” she said.
“I tried to use it to get away from my problems, but it made everything so much worse. When I was out with my friends partying and I was drinking and taking drugs, I felt great. I was taking so-called ‘party drugs’ like cocaine and ecstasy. But it was the come-down afterwards, when I had to face reality again and those suppressed feelings would hit me 10 times harder.”
During this period, Rachel, a former beauty student, said her relationship with drugs and alcohol “drove her into a darker place”.
She said the substance abuse was a weekly occurrence, and the mental consequences would linger until the following weekend, creating a cycle of rinse and repeat.
After a heavy night out and with no recollection of the incident, or the events leading up to it, Rachel attempted to take her life.
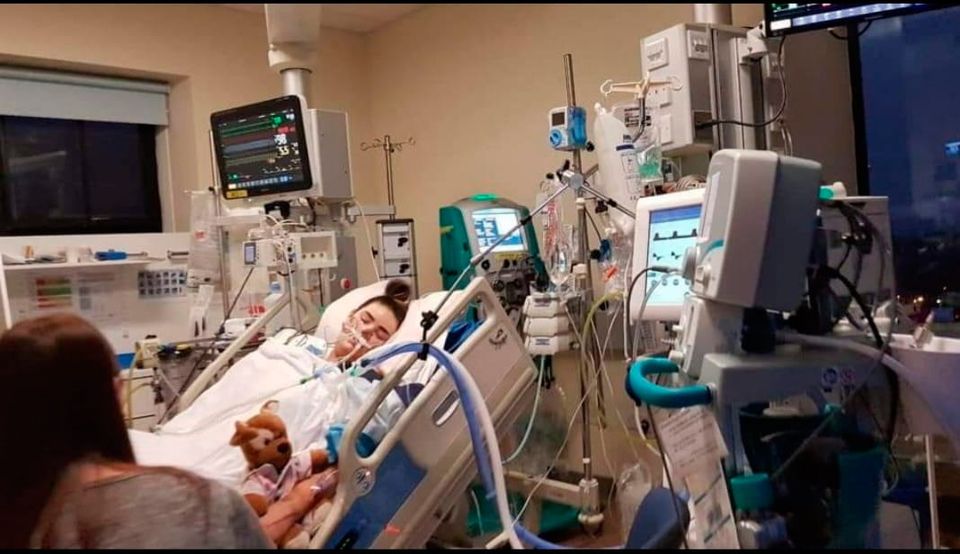
Rachel was left critically ill
“My mammy found me, and I was practically gone,” she said. “We had nurses that lived across the road from us at the time and one of them performed CPR on me for up to an hour, while waiting on the ambulance to arrive.”
Rachel was rushed to Altnagelvin hospital, where at one point her mother was told that due to her critical condition, there were no more available medical supports in Northern Ireland.
Her life support machine was due to be switched off, when an option became available, in Wythenshawe Hospital in Manchester, to receive extracorporeal membrane oxygenation (ECMO) treatment, which is not available in Northern Ireland.
“The hospital wasn’t sure that it would work due to my condition but thankfully they gave me a chance,” she added.
“My possibility of survival was at less than 1%. They came to the hospital in Derry and installed the machines, before transferring me to the hospital in Manchester. The aim of the treatment was to take over the function of my heart and lungs to give my body time for rest and repair.
“I spent around three weeks in Manchester. My condition started to improve, and it was on January 25 that they turned off the machine and found out I was going to make it.
“I remained in intensive care and was monitored for weeks following this, but this was a very promising sign.”
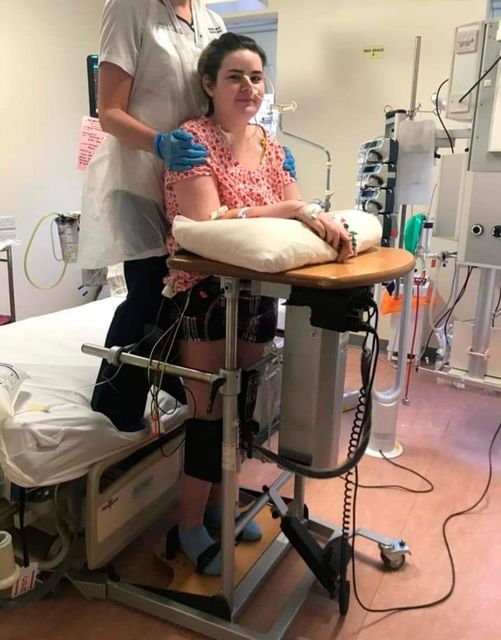
Rachel had to relearn basic tasks such as how to walk, talk and feed herself
Rachel recalls waking up from the coma and seeing her mother by her bedside. She credits her mum’s determination and the “fantastic staff” in both hospitals for her survival.
“I woke up in Manchester, normally patients don’t wake up there, so it was a shock to everyone that I did. I remember seeing my mammy — I do not know how she coped with it all.
“It was by complete luck that I was offered the treatment. Altnagelvin fought tooth and nail for me to get it. If it wasn’t for the consultant and the Manchester hospital giving me a chance, I would not be here today.”
Rachel had to “relearn all the basics”, through rehabilitation, such as how to walk, talk and feed herself.
Five years on, Rachel now faces the harsh reality of suffering from a chronic illness, and a hypoxic ischemic brain injury which prevents her from “living life as a typical 20-something”.
“Nearly five years sober from drugs and two years from alcohol, my health remains badly affected,” she said.
“I have a brain injury now and up until 2019 I was physically a healthy young girl. This has dramatically changed how I can live my life.
“There is no way of predicting my condition from one day to the next. My mobility has been affected, there are days that I rely on a walker or a wheelchair. I take seizures often that can be set off by a lot of things.
“I am still struggling to come to terms with my life now. Being 24 and everyone my age seems to be starting their careers, going out, and enjoying themselves — I can’t do that.”
Rachel hopes that by sharing her story, other young people will “reach out and seek help”.
She added: “I want to help people that are in a similar position I was in. I encourage them to reach out, speak to friends and family, talk to your GP about available support services— there is help there. Take action before it is too late.”
National Chung Cheng University of Crime Research Center - Education Center for Prevention of Drug Abuse
No.168, Sec. 1, University Rd., Minhsiung, Chiayi 621301, Taiwan 05 - 2724151 deptcrc@ccu.edu.tw
